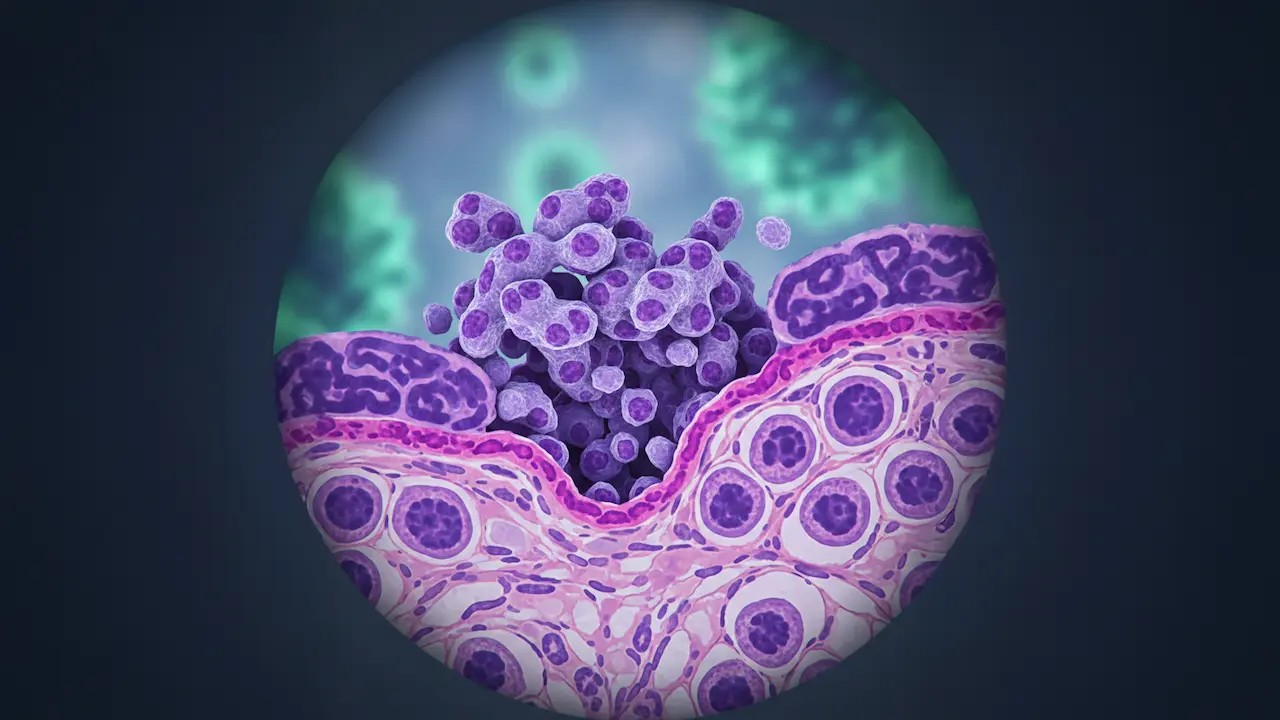
Cervical cancer is a biological process where cells in the lining of the cervix—the lower part of the uterus that connects to the vagina—undergo genetic changes that lead to uncontrolled growth. It is classified as a gynecological malignancy. In the vast majority of cases, this cellular transformation is initiated by a persistent infection with specific high-risk strains of the Human Papillomavirus (HPV).
In a healthy system, the cervix is composed of two main types of cells: squamous cells (on the outer part) and glandular cells (lining the canal). The “transformation zone,” where these two cell types meet, is the most common site for cancer to develop. The fundamental role of the cervix is to act as a gatekeeper between the vagina and the uterus; however, when its cellular replication cycle is hijacked by viral DNA, the tissue can transition from normal to precancerous (dysplasia) and, eventually, to invasive cancer.
Mechanism of Action: How it Develops
The progression of cervical cancer is typically a slow, multi-step process that occurs over several years or even decades.
- Viral Entry: The process begins when high-risk strains of HPV (most commonly types 16 and 18) enter the basal layer of the cervical epithelium through microscopic abrasions in the tissue.
- Viral Integration: Unlike many viruses that remain separate from human DNA, high-risk HPV can integrate its genetic material into the host cell’s genome. This allows the virus to produce specific oncoproteins, known as E6 and E7.
- Inhibition of Tumor Suppressors: The E6 protein binds to and degrades p53 (a protein that triggers cell death if DNA is damaged). Simultaneously, the E7 protein binds to and inactivates the retinoblastoma protein (pRb), which normally prevents cells from dividing too quickly.
- Uncontrolled Proliferation: With the “brakes” of the cell cycle removed, the infected cervical cells begin to replicate despite having damaged or mutated DNA.
- Cervical Intraepithelial Neoplasia (CIN): This stage represents the precancerous phase. Doctors categorize this growth as CIN 1, 2, or 3, based on how much of the epithelial thickness is affected.
- Invasion: If the immune system does not clear the infection and no medical intervention occurs, these abnormal cells eventually break through the “basement membrane” of the cervix, invading deeper tissues and potentially spreading to the lymph nodes or other organs via the circulatory system.
Historical Context
Cervical cancer has been documented since ancient times, but a major shift in understanding occurred in the late 19th and early 20th centuries. For many decades, it was one of the leading causes of cancer death for women globally. The most significant breakthrough came in the 1970s and 1980s when German virologist Harald zur Hausen identified the link between HPV and cervical cancer, challenging the then-prevailing theory that the Herpes Simplex Virus was responsible. This discovery fundamentally changed the field from one focused purely on surgical oncology to one focused on viral prevention and immunology, eventually leading to the development of the HPV vaccine.
Observed Data & Documented Findings
Global health data provides a clear picture of the behavior and prevention of this disease. According to the World Health Organization (WHO), cervical cancer is the fourth most common cancer in women worldwide.
Large-scale observational studies and clinical trials have established several key facts:
- Viral Correlation: Over 95% of cervical cancers are caused by the Human Papillomavirus.
- Screening Efficacy: In regions where regular screening (Cytology or HPV DNA testing) is implemented, the incidence of invasive cervical cancer has dropped by up to 70-80%.
- Vaccination Impact: Population-level data from countries with high HPV vaccination rates show a significant reduction in both the prevalence of high-risk HPV strains and the incidence of high-grade cervical lesions (CIN 3).
- Staging and Survival: Data from the National Cancer Institute (NCI) indicates that when caught at a “localized” stage (confined to the cervix), the five-year relative survival rate is approximately 91%. This rate decreases as the cancer spreads to regional or distant sites.
The Two-Sided View: Management & Prevention
Medical science approaches cervical cancer through two primary lenses: prevention (vaccination and screening) and intervention (surgery and radiation). Each pathway involves a balance of clinical outcomes and biological impacts.
| Potential Benefits (as reported in studies) | Reported Side Effects / Risks |
| HPV Vaccination: Highly effective at preventing infection from the most oncogenic strains of the virus. | Vaccine Reactions: Possible localized pain, redness, or syncope (fainting) immediately following injection. |
| Screening (Pap/HPV tests): Enables the identification and removal of precancerous cells before they become invasive. | Over-treatment: Procedures like LEEP or biopsies can sometimes lead to cervical scarring or a slightly increased risk of preterm birth in future pregnancies. |
| Surgical Intervention: Hysterectomy or trachelectomy can physically remove the primary tumor site. | Surgical Complications: Risk of infection, hemorrhage, or permanent loss of fertility (depending on the procedure). |
| Radiation/Chemotherapy: Effective at shrinking tumors and targeting cancer cells that have moved beyond the cervix. | Systemic Toxicity: Potential for fatigue, nausea, hair loss, and damage to surrounding pelvic organs (bladder or bowel). |
What We Know vs. What We Don’t Know
What science is confident about:
- High-risk HPV is the necessary cause of almost all cervical cancer cases.
- Regular screening significantly reduces mortality by catching the disease in the precancerous stage.
- The transition from infection to invasive cancer usually takes 15 to 20 years in individuals with normal immune systems.
What is still debated or unclear:
- The exact co-factors (such as smoking, long-term oral contraceptive use, or other co-infections) that determine why some people clear an HPV infection while others develop cancer.
- The optimal frequency and age-range for screening in vaccinated populations.
- Improving treatment outcomes for rare subtypes of cervical cancer, such as small cell neuroendocrine carcinoma, which do not follow the typical HPV-progression pathway.
References
Cervical Cancer – World Health Organization (WHO)
https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
Cervical Cancer: Statistics – American Society of Clinical Oncology (ASCO / Cancer.net)
https://www.cancer.net/cancer-types/cervical-cancer/statistics
HPV and Cancer – National Cancer Institute (NIH)
https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-and-cancer
Cervical Cancer Screening (PDQ®)–Health Professional Version – National Institutes of Health (NIH)
https://www.cancer.gov/types/cervical/hp/cervical-screening-pdq