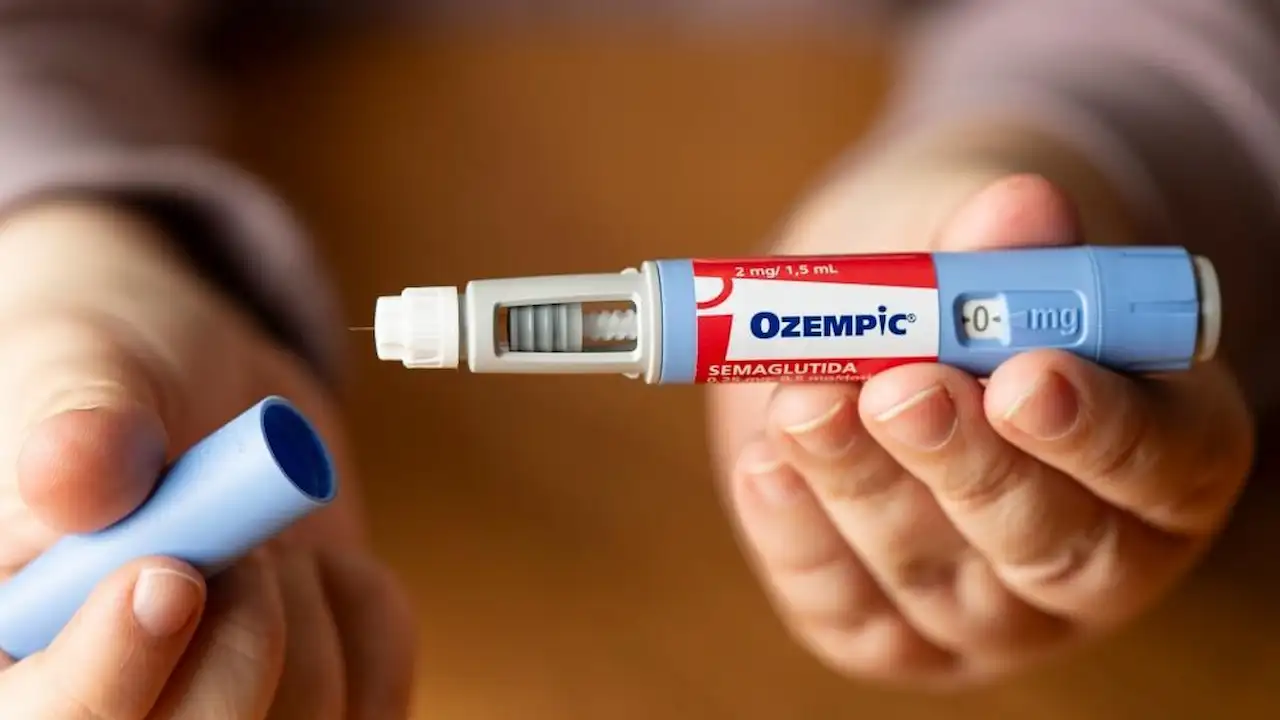
In the landscape of modern metabolic medicine, few substances have garnered as much public attention as Ozempic. Beyond the cultural discourse, Ozempic is a precise pharmacological tool designed to interface with the human endocrine system. Understanding its function requires looking past the trends and examining the biological mechanisms that govern how the body processes energy.
Objective Definition — What it is
Ozempic is the brand name for semaglutide, a medication belonging to a class of drugs known as glucagon-like peptide-1 (GLP-1) receptor agonists.
Technically, it is a synthetic analog of a naturally occurring hormone in the human body. It is primarily categorized as an incretin mimetic. Its fundamental role is to enhance the body’s natural response to food intake by regulating blood sugar levels and modulating appetite signals through the metabolic and neurological systems. While it is administered via a weekly subcutaneous injection, its primary site of action is at the molecular level, targeting specific receptors in the pancreas, liver, and brain.
Mechanism of Action — How it works
The “mechanism” of Ozempic is a multi-step process that replicates and extends a natural biological signal.
1. Hormonal Mimicry
When a person eats, the intestines naturally release a hormone called GLP-1. This hormone signals the pancreas to release insulin. However, natural GLP-1 is degraded by enzymes in the body within minutes. Semaglutide is engineered to be structurally resistant to these enzymes, allowing it to remain active in the system for approximately seven days.
2. Pancreatic and Hepatic Regulation
Once Ozempic enters the bloodstream and reaches the pancreas, it interacts with GLP-1 receptors on the beta cells. This interaction triggers two primary responses:
- Insulin Secretion: It stimulates the release of insulin, but notably, it does so in a glucose-dependent manner (meaning it primarily acts when blood sugar is high).
- Glucagon Suppression: It inhibits the release of glucagon, a hormone that normally tells the liver to release stored sugar into the blood.
3. Gastric Emptying
Ozempic acts on the digestive tract to slow down gastric emptying. This is the process by which food moves from the stomach into the small intestine. By prolonging the time food stays in the stomach, the medication induces a physical sensation of fullness (satiety) and prevents rapid spikes in blood glucose after a meal.
4. Neural Signaling
The medication crosses the blood-brain barrier to interact with the hypothalamus and other areas of the brain involved in reward and appetite regulation. It modulates the “hunger” signals, effectively lowering the biological drive to consume calories by increasing the threshold for satisfaction.
Historical / Development Context
The development of GLP-1 receptor agonists began in the late 20th century, following the discovery of the “incretin effect”—the observation that oral glucose causes a higher insulin response than intravenous glucose. Scientists became interested in semaglutide as a way to improve upon earlier GLP-1 medications (like exenatide or liraglutide) that required more frequent dosing. Ozempic was developed by the pharmaceutical company Novo Nordisk and received its first major regulatory approval for the treatment of Type 2 diabetes in 2017.
Observed Data & Documented Findings
The clinical profile of Ozempic is established through the SUSTAIN (Semaglutide Unabated Sustainability in Treatment of Type 2 Diabetes) clinical trial program, which involved thousands of participants globally.
- Glycemic Control: Data from the SUSTAIN trials consistently showed that a weekly 1.0 mg or 2.0 mg dose of semaglutide led to a significant reduction in $HbA1c$ (a measure of average blood sugar over three months), often reducing levels by 1.5% to 1.8%.
- Cardiovascular Outcomes: The SUSTAIN-6 trial focused specifically on cardiovascular safety. The findings indicated a 26% reduction in the risk of major adverse cardiovascular events (MACE), such as heart attack or stroke, in patients with Type 2 diabetes and high cardiovascular risk.
- Body Composition Changes: While Ozempic is indicated for diabetes, observational data across all trials noted weight loss as a primary secondary outcome. Study participants frequently lost between 5% and 15% of their total body weight depending on the dosage and duration of the study.
The Two-Sided View — Balance Table
The use of semaglutide involves a balance between metabolic regulation and systemic side effects.
| Potential Benefits (as reported in studies) | Reported Side Effects / Risks |
| Blood Sugar Reduction: Highly effective at lowering $HbA1c$ and maintaining glucose stability. | Gastrointestinal Distress: Nausea, vomiting, diarrhea, and constipation are the most frequently reported issues. |
| Cardiovascular Protection: Documented reduction in the risk of stroke and myocardial infarction in high-risk patients. | Gastroparesis: In some cases, the slowing of gastric emptying may become severe, leading to “stomach paralysis.” |
| Weight Management: Provides a physiological mechanism for weight reduction in individuals with obesity or diabetes. | Gallbladder Issues: Increased risk of cholelithiasis (gallstones) and cholecystitis (inflammation of the gallbladder). |
| Kidney Health: Some evidence suggests a protective effect on renal function in diabetic patients. | Pancreatitis Risk: A rare but serious potential inflammation of the pancreas has been observed. |
What We Know vs. What We Don’t Know
What science is confident about:
- Semaglutide is highly effective at mimicking the GLP-1 hormone and improving insulin sensitivity.
- The medication provides significant cardiovascular benefits for those with pre-existing heart conditions and Type 2 diabetes.
- The primary side effects are gastrointestinal and are often dose-dependent.
What is still debated or unclear:
- Long-term Maintenance: It is currently unclear how the body reacts to the cessation of the drug after multi-year use, specifically regarding “rebound” weight gain or metabolic resetting.
- Long-term Safety (Decades): While 5-10 year data exists, the impact of lifelong GLP-1 agonism starting in younger populations is still being monitored.
- Muscle Mass Loss: There is ongoing research into the ratio of fat loss versus lean muscle mass loss during rapid weight reduction on semaglutide.
References
Ozempic (semaglutide) Injection — Food and Drug Administration (FDA)
https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/209637lbl.pdf
Semaglutide and Cardiovascular Outcomes in Patients with Type 2 Diabetes (SUSTAIN-6) — New England Journal of Medicine (NEJM)
https://www.nejm.org/doi/full/10.1056/NEJMoa1607141
GLP-1 receptor agonists for the person with type 2 diabetes — National Institutes of Health (NIH)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10156073
Treatment of Obesity with Semaglutide — Mayo Clinic Proceedings
https://www.mayoclinicproceedings.org/article/S0025-6196(21)00346-6/fulltext