Legionnaires’ disease is a severe form of pneumonia—an inflammation of the lung typically caused by infection. It is categorized as a bacterial respiratory disease, specifically resulting from exposure to Gram-negative aerobic bacteria belonging to the genus Legionella. Within this genus, the species Legionella pneumophila is the most frequent causative agent in clinical cases.
Unlike many other respiratory pathogens, Legionella is not typically transmitted through person-to-person contact. Instead, it is an environmental pathogen that thrives in aquatic ecosystems. In the context of human biology, it is an opportunistic intracellular pathogen. It targets the lower respiratory tract, specifically the pulmonary alveoli, where it bypasses the body’s initial mechanical defenses to colonize cellular structures. Its presence triggers a systemic inflammatory response, disrupting the gas exchange function of the lungs and, in severe instances, affecting multi-organ homeostasis.
Mechanism of Action
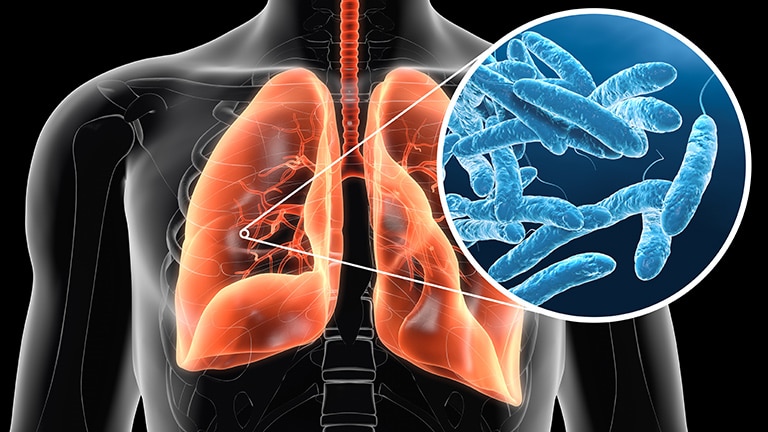
The progression of Legionnaires’ disease follows a specific biological sequence, from environmental colonization to cellular invasion.
Origin and Proliferation
Legionella bacteria exist naturally in freshwater environments like lakes and streams but become a human health concern when they colonize complex man-made water systems. These include cooling towers, large-scale plumbing systems, hot tubs, and decorative fountains. The bacteria proliferate within biofilms—slimy layers of microorganisms—where they are protected from standard disinfectants. They often survive by infecting and replicating inside single-celled protozoa (amoebae), which serve as their natural hosts in the water.
Pathway of Exposure
Human exposure occurs through the inhalation of aerosolized water droplets (mists) or, less commonly, the aspiration of contaminated water into the trachea. These microscopic droplets are small enough to bypass the upper airway’s cilia and settle deep within the lung’s alveolar sacs.
Cellular Interaction
Once in the alveoli, the bacteria encounter alveolar macrophages—immune cells designed to engulf and destroy foreign debris. Legionella has evolved a specialized mechanism called the Type IVB secretion system (T4BSS). Rather than being destroyed by the macrophage, the bacteria use this system to inject effector proteins into the host cell. These proteins redirect the cell’s internal trafficking, preventing the fusion of the phagosome with lysosomes.
Downstream Effects
The bacteria transform the macrophage into a “Legionella-containing vacuole” (LCV), a protected environment where they replicate rapidly. Eventually, the host cell ruptures, releasing a new generation of bacteria to infect adjacent cells. This process triggers a massive release of pro-inflammatory cytokines. The resulting inflammation causes the alveoli to fill with fluid and inflammatory debris (consolidation), significantly impairing the transfer of oxygen into the bloodstream.
Evolution of Understanding

The disease was first identified in 1976 following a large outbreak of respiratory illness among attendees of an American Legion convention in Philadelphia. The mysterious nature of the event prompted an intensive investigation by the Centers for Disease Control and Prevention (CDC), leading to the isolation of a previously unknown bacterium, subsequently named Legionella pneumophila. Since that discovery, scientific understanding has shifted from viewing it as a rare “outbreak” disease to recognizing it as a common, though underdiagnosed, cause of community-acquired and healthcare-associated pneumonia. Research has further evolved to focus on the complex relationship between the bacteria and man-made water infrastructure.
Observed Data & Documented Findings
Clinical data indicates that the severity of Legionnaires’ disease varies significantly based on host factors and the intensity of exposure. Large-scale observational studies conducted by public health agencies show that the incubation period typically ranges from 2 to 10 days, though some cases have documented windows up to two weeks.
Data from the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) highlight that certain demographics show higher susceptibility. These include individuals over the age of 50, current or former smokers, and those with chronic lung disease or compromised immune systems. Radiographic findings in confirmed cases usually show patchy or focal infiltrates that can progress to multi-lobar consolidation. Furthermore, clinical observations often note “extrapulmonary” symptoms—such as gastrointestinal distress (diarrhea) and neurological changes (confusion)—at higher frequencies than are seen in other types of bacterial pneumonia.
The Two-Sided View (Balance Table)
| Documented Observations / Clinical Characteristics | Reported Risks / Systemic Complications |
| Bacterial Clearance: Most cases are successfully treated with macrolide or fluoroquinolone antibiotics which penetrate host cells. | Antibiotic Resistance: While rare, some strains show reduced sensitivity to standard treatments in laboratory settings. |
| Diagnostic Accuracy: Urinary antigen tests provide rapid detection of L. pneumophila serogroup 1, the most common cause of illness. | Diagnostic Gaps: Standard urinary tests may miss other serogroups or species of Legionella, potentially leading to false negatives. |
| Environmental Control: Proper maintenance of water systems (thermal or chemical treatment) significantly reduces bacterial load. | Structural Persistence: Legionella can enter a “viable but non-culturable” (VBNC) state, allowing it to survive disinfection and reappear. |
| Immune Response: Healthy individuals often mount an effective immune response, sometimes resulting in a milder, non-pneumonic form (Pontiac Fever). | Organ Failure: Severe cases can lead to acute respiratory distress syndrome (ARDS), renal failure, or septic shock. |
Certainties vs. Variables
What science is confident about:
- Causative Agent: The genus Legionella is definitively established as the source of the infection.
- Transmission Mode: It is widely accepted that inhalation of contaminated aerosols is the primary route of entry into the human body.
- Intracellular Nature: The mechanism by which the bacteria subverts macrophages for replication is well-documented at the molecular level.
What is still debated or unclear:
- Low-Level Exposure: The exact minimum dose of Legionella required to cause infection in a healthy adult remains unquantified.
- Genetic Susceptibility: Why some individuals in the same exposure environment develop severe pneumonia while others develop mild Pontiac Fever or no symptoms at all is still being studied.
- Global Prevalence: Due to varying diagnostic standards and reporting requirements, the global burden of the disease is believed to be significantly higher than current official counts suggest.
REFERENCES
Legionella (Legionnaires’ Disease and Pontiac Fever) – Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/legionella/about/index.html
Legionellosis – World Health Organization (WHO)
https://www.who.int/news-room/fact-sheets/detail/legionellosis
Legionnaires’ Disease – Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/legionnaires-disease/symptoms-causes/syc-20351747
Legionella and Legionnaires’ Disease: 40 Years Later – Emerging Infectious Diseases Journal (CDC)
https://wwwnc.cdc.gov/eid/article/23/11/17-0402_article