1) Objective Definition — “What it is”
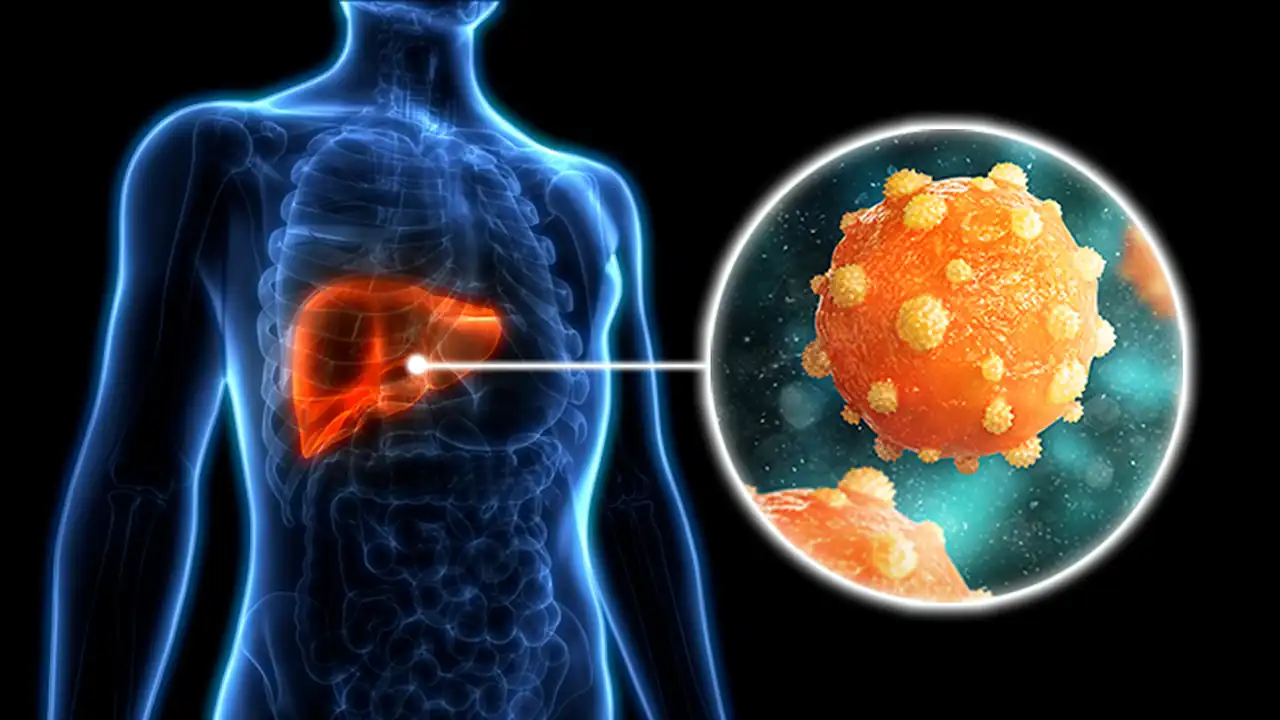
Hepatitis B is a systemic infection caused by the Hepatitis B virus (HBV), a small, enveloped DNA virus belonging to the Hepadnaviridae family. It is primarily a hepatotropic virus, meaning it specifically targets and replicates within the cells of the liver, known as hepatocytes. The liver is a vital organ responsible for over 500 functions, including protein synthesis, detoxification, and the production of biochemicals necessary for digestion.
Categorically, Hepatitis B is classified as a bloodborne pathogen. It is not a broad-spectrum condition but a specific viral entity defined by its genetic structure and its method of replication. Clinically, the infection is divided into two distinct states:
- Acute Hepatitis B: A short-term immune response occurring within the first six months of exposure. In many adults, the immune system successfully identifies and clears the virus during this phase.
- Chronic Hepatitis B: Defined by the persistence of the Hepatitis B surface antigen (HBsAg) for six months or longer. This occurs when the body’s immune system is unable to eradicate the virus, leading to a long-term presence in the liver.
Hepatitis B is characterized by its resilience; the virus is highly stable and can remain viable on environmental surfaces for at least seven days, maintaining its capacity to cause infection if it enters the bloodstream of an unvaccinated individual.
2) Mechanism of Action — “How it works”
The Hepatitis B virus operates through a complex, multi-stage replication cycle that distinguishes it from many other DNA viruses.
Step 1: Attachment and Entry
The process begins when the virus enters the bloodstream. It travels to the liver, where it recognizes and binds to the sodium taurocholate cotransporting polypeptide (NTCP) receptor on the surface of the hepatocyte. This receptor, which normally functions to transport bile acids, serves as the “lock” that the virus’s surface proteins “unlock” to gain entry.
Step 2: Uncoating and Nuclear Transport
Once inside the cell, the viral envelope is removed, and the viral core (capsid) is transported to the cell nucleus. The virus carries its genetic material in a form known as relaxed circular DNA ($rcDNA$).
Step 3: Formation of cccDNA
Inside the nucleus, the cell’s own repair enzymes convert the $rcDNA$ into covalently closed circular DNA ($cccDNA$). This $cccDNA$ acts as a stable “mini-chromosome” or reservoir. It is this specific form of viral DNA that makes Hepatitis B difficult to eradicate, as it persists in the nucleus even when viral replication is suppressed by medications.
Step 4: Transcription and Translation
The $cccDNA$ serves as a template for the cell’s machinery to produce viral messenger RNA (mRNA) and a specialized “pregenomic” RNA (pgRNA). These instructions are sent back out into the cell’s cytoplasm to build new viral proteins, such as the surface antigen (HBsAg) and the core antigen (HBcAg).
Step 5: Reverse Transcription and Assembly
In a unique biological twist, HBV uses an enzyme called reverse transcriptase to turn its pgRNA back into DNA inside new viral capsids. This is a characteristic usually associated with retroviruses like HIV.
Step 6: Release and Immune Response
The new viral particles are coated in a lipid envelope and released from the cell to infect neighboring hepatocytes. The actual damage to the liver is typically not caused by the virus itself, but by the host immune response. The body’s $CD8+$ cytotoxic T-cells recognize viral proteins on the surface of the liver cells and attack them to stop the infection, leading to inflammation (hepatitis) and, eventually, the replacement of healthy tissue with fibrous scar tissue.
3) Historical / Development Context
The identification of Hepatitis B was a landmark moment in 20th-century medicine. In 1965, Dr. Baruch Blumberg discovered an unusual protein in the blood of an Indigenous Australian person that reacted with the serum of a patient with hemophilia. He initially named this the “Australia Antigen.” By the late 1960s, researchers linked this antigen specifically to “serum hepatitis” (as opposed to “infectious hepatitis” or Hepatitis A). This discovery allowed scientists to develop the first diagnostic tests to screen the blood supply and eventually led to the development of the first plasma-derived vaccine in 1981, followed by the recombinant (genetically engineered) vaccine in 1986. Dr. Blumberg was awarded the Nobel Prize in Physiology or Medicine in 1976 for this work.
4) Observed Data & Documented Findings
Global health data provides a quantitative look at the behavior and impact of HBV:
- Global Prevalence: According to the World Health Organization (WHO), an estimated 254 million people were living with chronic hepatitis B infection as of 2022. The highest prevalence is observed in the African and Western Pacific regions.
- Transmission Efficacy: Clinical studies have documented that HBV is 50 to 100 times more infectious than HIV. While both are bloodborne, HBV requires a much smaller viral load to establish an infection in a host.
- Chronicity and Age: Data shows a direct correlation between the age at infection and the risk of chronicity. Approximately $90\%$ of infants infected at birth develop chronic infections, whereas only $5\%$ of healthy adults who contract the virus will fail to clear it naturally.
- Liver Complications: Longitudinal observational studies indicate that without clinical management, approximately $20\%$ to $30\%$ of adults with chronic HBV will develop cirrhosis or hepatocellular carcinoma (liver cancer).
- Vaccine Impact: Since the implementation of universal infant vaccination programs, the prevalence of HBV among children under five years of age has dropped to less than $1\%$ globally, compared to approximately $5\%$ in the pre-vaccine era.
5) The Two-Sided View — Balance Table
The management and prevention of Hepatitis B involve weighing different clinical realities.
| Potential Benefits (as reported in studies) | Reported Side Effects / Risks |
| Vaccination: Provides a high level of protection (95% efficacy) against infection and subsequent liver cancer. | Injection Site Reactions: Common side effects include localized soreness, redness, or swelling at the injection site. |
| Antiviral Suppression: Medications (like Tenofovir or Entecavir) effectively lower the viral load in the blood, slowing liver damage. | Lifelong Commitment: Most current antiviral treatments do not provide a “cure” and must be taken indefinitely to prevent viral rebound. |
| Natural Immunity: 95% of healthy adults clear the virus and develop lifelong protective antibodies (anti-HBs). | Immune-Mediated Damage: The body’s attempt to clear the virus can cause acute liver failure in rare, severe cases (fulminant hepatitis). |
| Perinatal Prevention: Administering the vaccine and immunoglobulin at birth prevents 90% of mother-to-child transmissions. | Access Disparity: High-cost interventions and diagnostics remain unavailable in many high-burden, low-resource settings. |
6) What We Know vs. What We Don’t Know
What science is confident about:
- Modes of Transmission: We know the virus is spread through blood, semen, and vaginal fluids. It is not spread by sharing utensils, breastfeeding, or casual contact.
- Detection: Standard blood tests can accurately distinguish between a current infection, a chronic state, and immunity (either from past infection or vaccination).
- Vaccine Safety: The Hepatitis B vaccine has one of the longest and most robust safety records of any modern immunization.
What is still debated or unclear:
- The “Functional Cure”: While we can suppress the virus, we do not yet have a reliable way to eliminate $cccDNA$ from the liver cells entirely.
- Immune Tolerance Phase: The exact mechanisms that determine why some individuals remain “immune tolerant” (high virus levels but low liver damage) for decades while others progress rapidly is still under investigation.
- Reactivation Triggers: Why the virus suddenly “wakes up” and causes liver damage in dormant carriers, especially during unrelated immunosuppressive treatments, is not fully understood.
REFERENCES
Hepatitis B Key Facts — World Health Organization (WHO) https://www.who.int/news-room/fact-sheets/detail/hepatitis-b
Hepatitis B Questions and Answers for the Public — Centers for Disease Control and Prevention (CDC) https://www.cdc.gov/hepatitis/hbv/bfaq.htm
Hepatitis B Virus Infection — Nature Reviews Disease Primers https://www.nature.com/articles/nrdp201835
Hepatitis B — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) https://www.niddk.nih.gov/health-information/liver-disease/viral-hepatitis/hepatitis-b